The Healthy Heartbeat - Volume 4
Atrial Fibrillation (AFib): The Most Common Arrhythmia
Abnormalities in the heart’s electrical system can cause the heart to beat too slowly, too quickly, or erratically. These abnormal heartbeats are known as arrhythmias. The most common arrhythmia, atrial fibrillation (AFib) affects 3 to 6 million Americans—almost one in 10 people over the age of 65! Here are some essential facts to help you stay aware of this condition so you can stay healthy and in rhythm.
As your heart beats, the top chambers of the heart, or atria contract and push blood into the bottom chambers, or ventricles. In atrial fibrillation, the stimulation of the atrial chambers becomes extremely rapid due to abnormal electrical triggering from the pulmonary veins. As a result, the chambers “quiver” rather than squeeze blood. Clot formation and strokes can result, as well as abnormally fast or uncoordinated heart beats. AFib can occur in brief episodes, frequently, or become a permanent condition.
Did you know? Untreated, atrial fibrillation doubles the risk of heart related deaths and means a four to five times higher risk of stroke!
AFib Symptoms
About one-third of people affected do not have any symptoms and are diagnosed with AFib incidentally. Other people demonstrate any of a number of symptoms, including rapid, pounding, or erratic heartbeat, weakness, shortness of breath, extreme fatigue, and in some cases chest pain. Sometimes people feel a sense of just “not feeling right” and can vaguely perceive that their heart rhythm is just not in sync.
Risk Factors for AFib
- Age. Although young people can develop AFib, incidence increases with age
- High blood pressure
- Obesity
- Diabetes
- Heart failure
- Ischemic heart disease
- Hyperthyroidism
- Chronic stress
- Excessive alcohol intake (more than 1 drink a day for women and 2 drinks a day for men)
AFib Treatments
The symptoms of AFib are usually treated by restoring the normal heart rhythm, and preventing future episodes from being triggered. We call this “rhythm control”. This strategy is usually employed alongside protecting you from stroke.
The treatment that is most appropriate for you will depend on how long you've had atrial fibrillation, the extent of your symptoms, and the underlying cause. It’s best to go through all of the options with your cardiologist or heart rhythm specialist (cardiac electrophysiologist). Below is a brief description of the types of treatments that are often chosen.
Sometimes an initial strategy is to “reset the rhythm” with something called a cardioversion. This usually temporarily restores the rhythm to normal, but does not prevent future episodes of AFib. Therefore, it is usually paired with another strategy to keep the rhythm normal. Sometimes this can be accomplished with medication and lifestyle changes, and other times the better option is to pursue a procedure called catheter ablation.
Catheter Ablation
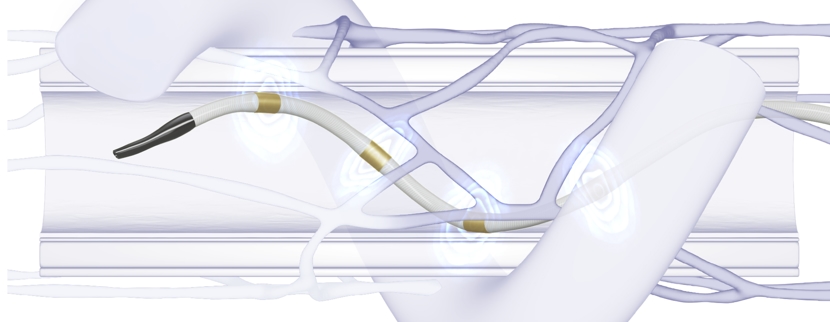
Catheter ablationis a procedure performed by an electrophysiologist. This minimally invasive procedure destroys tiny areas of abnormal electrical tissue through freezing (cryoablation) or cauterization/burning/”zapping” (radiofrequency ablation). Catheter ablation is a highly effective and safe procedure. With recent advances in experience and technology, almost all patients have a dramatic reduction in the amount of AFib they have, and some of them are effectively cured.
We now know that early treatment of AFib prevents progression to more severe or entrenched forms. With any diagnosis of AFib, a cornerstone is to see your cardiologist or cardiac electrophysiologist to discuss these treatment options.
For these reasons, patients are increasingly reaching for catheter ablation as an early strategy to prevent worsening of AFib, fix their symptoms, and return to an active lifestyle. MarinHealth Medical Center’s new Oak Pavilion features a brand new electrophysiology suite. Speak with your cardiologist to learn about options and the latest technology.
Stroke Risk and Percutaneous Left Atrial Appendage Occlusion
Clots in AFib most often form in a structure called the left atrial appendage, a “blind alley” where blood tends to stagnate. Often, we prescribe blood thinners to reduce the potential for clot formation. Unfortunately, these medications are not a good fit for everyone since they can increase propensity for bleeding. We often seek an alternative, either due to side effects, bleeding, an active lifestyle that increases risks of serious injury, inefficacy, or a patient’s desire to seek an alternative to blood thinners.
We now have access to a highly effective procedure called percutaneous left atrial appendage occlusion. This involves inserting a small device (with an FDA approved device called the WATCHMAN™ FLX, often leading to the alternative term “WATCHMAN™ procedure”). This procedure is percutaneous (minimally invasive), and involves placing this mini umbrella into the left atrial appendage. The procedure is done under general anesthesia and typically takes about an hour. After the procedure, patients usually spend one night in the hospital before being discharged. The WATCHMAN™ device serves as a scaffold for your body to grow a “skin” over the surface of the device, reducing the potential for embolism from the appendage. Our data shows that most patients can very effectively be protected against stroke, and >95% are able to discontinue their blood thinners after this procedure.
MarinHealth Medical Center was one of the first hospitals in the nation to be granted use of the original WATCHMAN™ implant, so our team of experts has extensive experience using this innovative treatment. We are one of the Bay Area centers of excellence for this procedure. Learn more about the WATCHMAN™ procedure and benefits.
Staying on the Forefront: MarinHealth Electrophysiology Research
As a leading-edge provider of advanced technology and novel electrophysiology interventions, MarinHealth’s electrophysiology team is committed to participating in research studies, with single-center and multicenter clinical trials. In addition to advancing medical science, these trials allow us to offer our patients innovative treatments that are typically only available through an academic hospital. Please contact your cardiologist, or call 1-415-927-0666 to speak with the site primary investigator, Vivek Iyer, MD, and research coordinator, Liliana Espinosa Bonell, if you are interested in participating in any of these exciting trials.
We are currently enrolling patients in multiple trials, including but not limited to the following:
- PLEA-AF: Investigating the ideal strategy for ablation of persistent atrial fibrillation,
- OPTION: Evaluating the optimal mode of stroke prevention post ablation of atrial fibrillation, with anticoagulation or percutaneous left atrial appendage occlusion with the WATCHMAN™ FLX device,
- CHAMPION: Comparing outcomes in patients randomized to receive percutaneous left atrial appendage occlusion or ongoing blood thinners,
- SYNC-AV: Studying cardiac pacemaker settings for resynchronization of the heart.
Don’t wait another beat. If you have concerns about AFib or another arrhythmia, call 1-415-927-0666 to request an appointment with one of MarinHealth’s expert electrophysiologists. Most appointments will be scheduled within 48 hours.
Jake Peterson: AFib Care at MarinHealth Medical Center
Jake Peterson was just 29 years old the first time his heart went into atrial fibrillation. As a young and healthy fire captain, he was surprised to learn just how common AFib is in younger people. Learn more about the treatment Jake received, and the changes he has made to protect his health, including participating in Get into Rhythm, a lifestyle program at MarinHealth designed specifically for atrial fibrillation patients.
Is Learning to Relax Easier Said than Done?
No matter how you slice it, stress can be bad for the heart. We all experience stress, which can be beneficial short-term, such as giving us the boost we need to deliver a presentation or meet a tight deadline. But when stress is constant, it can impact sleep, weight, blood sugar—and just about every metric associated with heart disease, from blood pressure to high cholesterol. The problem is that most of us are so chronically stressed that we don’t always recognize the signs and symptoms. But if you’ve been diagnosed with AFib—or any heart disease really—learning how to stay calm and manage your stress will be an important part of your treatment and ongoing management. Even if you don’t have any heart health concerns, learning to identify stress triggers, relax, and take time to find some calm and quiet in your regular routine is a great way to protect your heart and overall health.
Setting boundaries at work, spending time with friends and loved ones, exercising, and making time for the hobbies and activities you love, whether playing the piano or sitting on the beach, are all good tips. But if you have AFib or are looking to reduce your risk of heart disease, setting aside some time everyday devoted just to your health and wellbeing is critical. A few minutes of meditation or guided relaxation can be done just about anywhere, even when you only have a few minutes to spare. It doesn’t require any special equipment or training, and although you can take a class to learn the basics, you can also practice on your own without spending a dime!
The research on meditation is clear, and the health benefits are considerable. With regular practice, studies have shown that meditation can help:
- Slow your breathing and immediately improve your sense of calm
- Reduce blood pressure
- Help manage irritability and moodiness
- Help alleviate pain
- Reduce anxiety and depression
- Improve sleep
- Reduce risk for some cancers
- Improve attention and concentration
If you’re new to meditation, it might be helpful to start with a few guided meditation and relaxation exercises. In fact, even those who have been practicing meditation for years may find that listening to podcasts or videos can be very helpful. Try a few different options and see what works for you. MarinHealth has a series of guided meditations that range from about 30-45 minutes, and they are free to access on our YouTube channel. We also offer free, weekly virtual meditation classes.
There are also a multitude of meditation apps available, some with subscription fees such as Calm, and others that are free of charge like Insight Timer. Try a few and you’re sure to find something that’s right for you. If carving out 30 minutes is a challenge, start small—even a 5- or 10-minute meditation can make a big difference.
And when you’re really in a crunch and need a quick calming fix, just find a quiet place, close your eyes for a few minutes, and practice breathing in and out slowly and deeply from your abdomen. There are several different “patterns” you can try, but the simplest one is to simply breathe in while you slowly count to four, then exhale while you again count to four. Or try the 4-7-8 method: breathe in for a count of four, hold while you count to seven, then slowly exhale while you count to eight. Repeat as many times as possible, but even just four or five repetitions should give you more control over your breath and leave you a little more relaxed.